Surgical complications and pitfalls in taTME
Introduction
Transanal total mesorectal excision (taTME), provides a unique approach to difficult rectal dissection by bringing the low pelvis closer to the operating surgeon. This has led to impressive early outcomes in phase 2 and registry studies (1). However, any new technique comes with a learning curve, where the risk of complications is potentially increased. taTME brings a change of perspective to pelvic anatomy that is unfamiliar to colorectal surgeons, which has led to distinct complications such as the notorious urethral injury (2,3). Pneumodissection caused by the insufflation of pelvic surgical planes also adds to the possible confusion. Urethral injury, of course, is not the only pitfall that may result. Fecal contamination, wrong plane surgery leading to violation of the mesorectal fascia or rectum, injury to splanchnic and inferior hypogastric plexus and branches, lateral side wall injury, posterior sacral injury leading to bleeding, carbon dioxide embolism and anastomotic failure are other possibilities. Granted low anterior resection, using any technique, has repeatedly demonstrated complications in nearly one-third of patients. Nonetheless, now that the approach celebrates its tenth anniversary, techniques have been developed to avoid and minimize these potential pitfalls. This article seeks to guide the read through these pitfalls and techniques to reduce their occurrence. Nonetheless, formal teaching, simulation, proctoring and team training still play an important role in processing the inevitable learning curve of taTME.
Pursestring failures
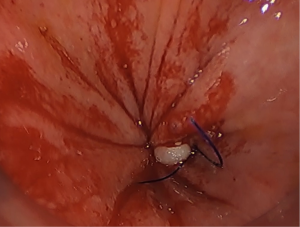
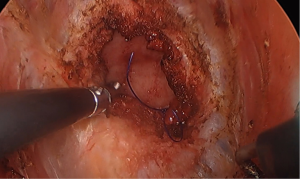
One of the most important steps, and specifically unique to taTME, is the application of the initial pursestring. The initial pursestring, assures a negative distal margin, avoids proximal distention of the colon, and facilitates pelvic dissection by maintenance of “pneumopelvis”. Failure to completely secure an proper pursestring (Figure 1) leads to bacterial or gross fecal contamination of the surgical field, making the operation more difficult and heightening the risks of other possible injuries. Crucially, seeding of tumor cells may result from this spillage, potentially increasing the risk of local recurrence. Perforation of the rectum in traditional TME is well known to increase rates of local recurrence (4), and spillage of fecal and tumor cells is likely to have the same result.
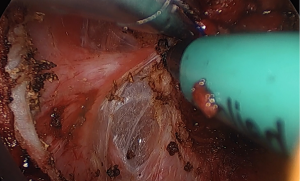
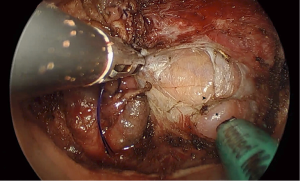
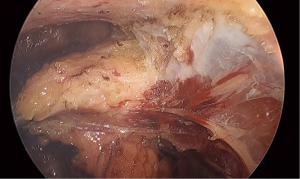
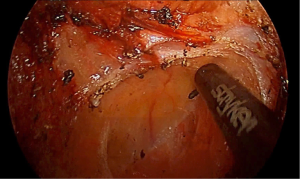
The mainstay preventative measure is to ensure that the pursestring is constructed correctly. The first step is to mark the proposed pursestring site with cautery. Transanal suturing is unfamiliar to most surgeons, and often requires a high level of mental attention due to its difficulty (5). Spiraling the pursestring, which usually occurs when the anterior sutures are placed more proximally, has been observed frequented both in cadaveric training and live surgery, which leads to an insecure or asymmetric pursestring. The avoidance of long travel on each bite will also reduce the possibility of a defect within the pursestring. A full-thickness bite that takes the longitudinal muscle of the rectum is ideal; too deep and the suture may obscure dissection planes as it draws in surrounding tissues (Figure 2). Too superficial, and the suture may end up ‘cutting out’, acutely opening up the rectum. It is preferred to tie the pursestring in an open fashion, with the cap of the port off, either by hand or with a knot pusher, to ensure the pursestring is tight. Finally, checking the pursestring by attempting to pass a forceps should be performed prior to insufflation. If any defect is found, this may be remedied with figure-of-eight sutures, or cutting out the pursestring and redoing it. Pursestring failure after the dissection has commenced can often be rescued by the application of an endoloop. Following closure of the pursestring, repeating the washout of the surgical field with betadine or chlorhexidine should be performed. It is essential that the surgeon is satisfied with the quality of the pursestring as this will avoid potential catastrophe later (Figure 3).
Wrong plane surgery
As with any other aspect of colorectal surgery, wrong plane surgery often leads to injury to surrounding organs, and neurovascular structures. Identification of the multiple planes of the rectal wall and pelvis following proctectomy and exacerbated by the effects of pneumopelvis is unfamiliar to surgeons. Although nothing can substitute from careful observation, supportive supervision and experience, the authors believe that the following guides will help surgeons avoid wrong plane surgery and remain in the correct surgical plane.
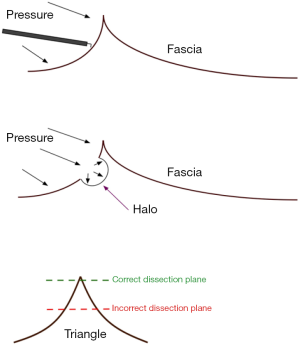
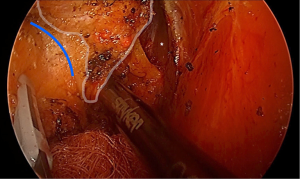
It is vital that the TME dissection is performed circumferentially equally and that uneven progress is not made in one sector over the others. If uneven dissection is performed, the pneumorectum will unevenly push the specimen away and distort the contralateral planes, leading to dissection that is either too shallow of deep. Traction on the tissue, as always, is enormously important to correct plane surgery, and dissection should not proceed without proper tension. Another clue is to look for ‘triangles and ‘Os’, which have been described in detail, and result from the effects of insufflation and retraction during surgical dissection (Figure 4) (6). The correct plane is found at the tip of the ‘triangle’ that is formed when tissues are placed on stretch (Figure 5). Once the tip is dissected, the plane can be continued along the border of the ‘triangle’. If, at any point, an ‘O’ sign is encountered, this indicates that new plane of dissection has been entered (Figure 6). Rarely is this an indication of the correct plane. More commonly, it marks a plane that is too deep, and that continuing in this plane will endanger pelvic side wall strictures or pelvic veins. Lastly, encountering bare muscle at any point is an indication that the plane is too deep. Even in the skinniest patients, there is a thin layer of endopelvic fascia that will lie upon the pelvic floor or muscles of the pelvic side wall (Figure 7).
Pelvic nerve injury
The lower third of the rectum is innervated by a complex network of autonomic nerves composed of the superior hypogastric plexus comprised by sympathetic nerves, the inferior hypogastric plexus comprised of sympathetic and parasympathetic nerves, and the pelvic splanchnic nerves. During dissection of the infraperitoneal rectum, the autonomic nerves and plexuses are at high risk of injury especially during dissection of the rectum from the prostate, seminal vesicles, and vagina. Nerve injury during total mesorectal excision, occurs most commonly from excessive lateral dissection, extramesorectal dissection, and additionally retraction injury. Urologic and sexual outcomes have been studied extensively in open, laparoscopic, and robotic surgery with a wide range of reported dysfunction, 11-85%, and overall equivalence between techniques (7,8). The majority of cohort studies demonstrate strong selection bias, however, and furthermore, include learning curves during the adoption of minimally invasive surgery over the last two decades. A single randomized trial in a small cohort of distal third rectal cancers, by Denost et al. (9) suggested superior outcomes of sexual function favoring the transanal approach.
TaTME leaves the autonomic plexus similarly vulnerable to nerve injury as previous techniques. Although enthusiasts and early adopters often cite improved visualization, superior access, and easier retraction as to why nerve injury may be less likely, the mechanics of extrarectal pneumodissection, combined with the difficulties of a novel anatomic approach and the requirement of advanced minimally invasive skills may leave the nerves even more susceptible to damage, especially early in the learning curve. A thorough understanding of the nerve distribution seen from the transanal approach, combined with precise mesorectal dissection, is critical to avoid unnecessary nerve injury and resultant impaired functional outcomes from poor surgical technique. The superior hypogastric plexus and nerves are only involved during the abdominal portion of taTME and are of no concern during transanal dissection.
The pelvic splanchnic nerves are composed of the anterior rami of sacral nerves 2−5 and provide parasympathetic innervation to the hindgut. Their initial course lies deep to the parietal fascia, however, as they ascend to join the inferior hypogastric plexus, they pierce the endopelvic fascia and ultimately cross the retrorectal space to form branches into the rectum through the lateral ligaments. During taTME, the lower splanchnic nerves are commonly susceptible to injury during the initial dissection and identification of the appropriate mesorectal plane. Following full thickness proctotomy, clear recognition of the endopelvic fascia at the 4 and 8 o’clock position with dissection within avoids early lateral exposure of the splanchnic nerves. Visualization of the bare red muscle fibers of the levator ani muscle is the earliest clue that dissection has proceeded deep to the endopelvic fascia, placing the nerves at risk (Figure 8). Further mobilization cephalad requires dissection just on the fascia propria of the rectum to avoid injury to the nerves as they lay on top of the endopelvic fascia and are often tented in by the retracted rectum (Figure 9).
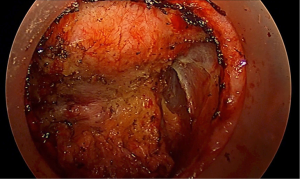
The inferior hypogastric plexus in the lower third of the rectum is formed from a coalescence of distal afferent fibers from the sympathetic hypogastric trunks, as they descend, and pelvic parasympathetic fibers from the splanchnic nerves. Fibers from the inferior hypogastric plexus innervate the seminal vesicles, prostate, bladder, cervix and vagina. These nerves are responsible for penile erection, detrusor contractility, female arousal, and vaginal lubrication. Dissection of the extraperitoneal rectum too laterally during conventional TME has been well described as a cause of plexus injury and sexual dysfunction. With taTME, excessive lateral dissection is a common occurrence, especially early in the learning curve, exposing the plexus to increased injury. Dissection often can proceed unnoticed well up the sidewall of the obturator internus, lateral to the pelvic plexus and obturator nodal packet. During corrective maneuvers to adjoin with the anterior plane, the entire neurovascular bundle is at risk for transection (Figure 9). Dissection anterior to Denonvillier’s fascia, classically described by Heald, is also speculated to increase risk of nerve injury and has evolved to selectively dissect posterior to the fascia based on tumor location and concern over circumferential resection margins. Similarly, during taTME, the surgeon can choose the appropriate level of dissection, taking special caution anterolaterally where the neurovascular bundles (of Walsh) are more anatomically accessible.
Vascular injury
Injuries to vascular structures with resultant bleeding is a risk with any surgical procedure and have been well described in traditional TME. The same vessels encountered in both the appropriate TME plane and inadvertent extramesorectal plane are similarly vulnerable during transanal TME. In general, the proximity to the vessel and angle at which it is approached from the transanal viewpoint permits easier identification and control. As a rule, the vessel should be handled from the same trajectory as the occurrence, thus attempting to control from the top is more challenging with inferior exposure.
As with the conventional approach, injury to the presacral plexus of veins, deep to the presacral fascia is not uncommon and often occurs at the same location. Failure to follow the acute curvature of the sacrum with proximal dissection takes one deep to presacral fascia.
Direct compression with a dry guaze for several minutes or bipolar cautery is easy from this orientation. Dissecting just on the mesorectal envelope is critical to avoid this mishap.
Waldeyer’s fascia is an important landmark around S3, and must be divided to continue in the normal plane. Failure to appreciate this subtlety will quickly force the plane towards and sometimes through the presacral fascia.
The middle rectal arteries, described coursing within the lateral stalks, vary in their origin, independence, and true presence. Anatomical studies demonstrate presence of bilateral middle rectal arteries as little as 12% of the time. When present, nearly 70% have a common origin with prostatic arteries forming a large prostate-rectal trunk. During traditional TME, they are often handled with impunity, divided without clear visualization using advanced bipolar energy or more commonly with simple monopolar cautery. From the transanal approach, they seem to appear with increased clarity requiring definitive treatment (Figure 10). Most commonly, exposure is facilitated by the transanal team, permitting easy access and division by the abdominal team with bipolar energy during synchronous taTME.
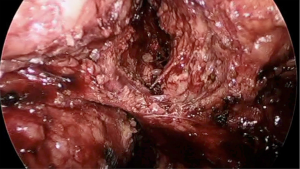
The remaining causes of vascular injuries generally occur from inappropriate extramesorectal dissection, usually from inadvertent lateral dissection where venous and arterial branches of the terminal internal iliac branches are found. Additionally, extramesorectal vasculature can be injured from tenting in during retraction, especially the anterior arteries supplying the urogenital organs which can be easily manipulated to assume a more perpendicular orientation.
Lateral side wall injury
In the earliest days of taTME, the pelvic side wall was often entered inadvertently. Fears of not impinging on the TME specimen, as well as the natural tendency to dissect outwards from the narrowest point of the distal pelvis led to extramesorectal dissection. Subsequent analysis of cases, as well as the pioneering work being done in Japan into transanal lateral lymph node dissection (TaLLND), has provided insights into this phenomenon.
It is at the level of the seminal vesicles that the lateral side wall is most easily entered. A pillar of extramesorectal fat exists here (Figure 8) that marks possible entry into the side wall structures. Dissection lateral to this pillar will lead to the obturator lymph node space which is usually dissected in pelvic lymphadenectomy. Recognizing this, even only in hindsight once the space has been opened, is an important marker to avoid side wall injury. Laterally, the exposure of the bare surface of obturator internus, should be a danger, marking that the pelvic side wall has been entered. Reestablishing the correct plane following the appropriate curvature of the mesorectum, and displacing the plexus proximal and laterally is crucial. Fortunately, as long as only a small amount of the surface obturator internus is exposed, and the dissection is not continued, there should be no injury to the vital side wall structures. Proximally in the obturator space the obturator nerve is encountered in addition to the obturator artery and vein. Posteriorly, in the obturator space, the distal branches of the internal iliac, the inferior gluteal and pudendal vessels can cause severe bleeding just before passing through Alcock’s canal.
Carbon dioxide embolism
Carbon dioxide, air, or gas embolism, once most commonly identified during laparoscopic liver surgery, has been increasingly acknowledged during taTME. Its occurrence during conventional transabdominal minimally invasive TME is nearly unheard of. Gas embolism is a life-threatening sequelae is marked by a drop in end tidal CO2, O2 saturation, followed by hypotension and then asystole. This was most recently described in a recent publication in Diseases of the Colon & Rectum by the taTME working group which described 25 cases (10). Use of the Airseal (Conmed Surgical, Denver, Colorado)insufflation system was present in 24 of the 25 cases, although the vast majority of cases in the entire registry are performed with Airseal. A bleeding site was identified in 21 of the cases, and in 40%, it was due to a periprostatic vein. In addition, an additional 12% of cases were due to a vaginal vein injury. Therefore, the majority of injuries occurred when a large anterior vein was disrupted. In 28% of further cases, other pelvic veins were injured. It is postulated that the positive pressure from the pneumorectum pushes CO2 into the venous system, creating the embolus. No deaths have been reported from gas embolism, however, cessation of the operation with subsequent delayed completion is not an unreasonable result.
An acute drop in end tidal carbon dioxide monitored by the anesthetist is often the first and most obvious clinical indicator of gas embolism and should not be ignored. Immediate management should include stopping all CO2 insufflation, control of the bleeding directly or with packing, flooding the field with normal saline, ventilation with 100% oxygen and circulatory support. Other measures should include insertion and aspiration of a central venous catheter, cardiopulmonary resuscitation and hyperbaric oxygen. Prevention is the best solution, with quick control of any bleeding, and consideration for lowering the CO2 insufflation when there is any hemodynamic concern. In addition, education of our anesthetic colleagues to its possibility will facilitate by preparation and prompt diagnosis.
Urethral injury
Urethral injury is probably the most feared of the possible complications from taTME, likely due to its impossibility during conventional low anterior resection, challenges to repair, and the seriousness of long-term sequelae. Injury to the urethra has been described in the literature previously during the perineal phase of abdominoperineal resection, however, it would appear to be quite rare (11). Apart from having prescience that this risk exists, the most helpful sign is the presence of striated muscle in addition to bleeding during the anterior dissection. This should always prompt careful re-evaluation of the current progress in the operation. Use of energy devices should be extremely judicious, and only used to stop the current bleeding rather than continuing the dissection.
The urethra lies anterior the prostate, which encompasses it from behind. Therefore, injury to the urethra absolutely requires improper dissection anterior to the prostate, first dropping the prostate down, and subsequently, forcing the distal membranous urethra to assume a vertical orientation. For this reason, the authors have adopted an anterior first approach allowing early identification and entry into the rectoprostatic plane. In addition, dissecting posteriorly first, and then following the plane laterally to finish anteriorly can lead to prostatic mobilization by initial excessive lateral dissection. Be wary of encountering any large vascular structures, as the anterior mesorectum is usually quite thin, even in obese patients, and rarely has large vessels within it. Observation of this should prompt immediate caution. In the same vein, the presence of a bulky midline structure should be immediately alarming and prompt immediate reflection (Figure 11).
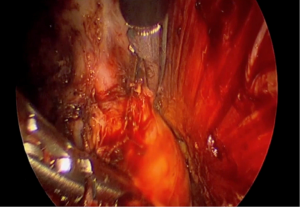
Urethral injury is much more likely to result from intersphincteric dissection of distal rectal tumors, as plane identification, and dissection deep and too lateral to the endopelvic fascia is more common. Radiation induced fibrosis and edema, as well as anterior tumors increase difficulty. At this level, the mesorectum is absent and requires dissection directly on the anorectal tube. Dissection too anterior, leads to early mobilization of the prostate, thus dropping it down. The use of illuminated ureteral catheters, indocyanine green, and frequent palpation or manipulation of the urinary catheter have all been utilized to maintain orientation and avoid urethral injury (12,13).
Anastomotic failure
A review of the international taTME registry, recently suggested increased rates of anastomotic leak following taTME (14). Although this certainly reflects the learning curve and early adoption of taTME, two principal factors are unique to taTME and account for the change in technique required for successful anastomosis. First, following specimen extraction, an open anorectal cuff remains and requires secure transanal closure. Secondly, a secure pursestring closure will still leave a small central defect, as it is not secured around a stapler anvil as with the traditional technique.
Ensuring complete mobility of the distal rectal stump is felt to be important. If the stump is fibrotic or immobile due to fixation of surrounding tissues, adequate securing of the pursestring can be more challenging, leaving a much larger central opening for the anvil, and increasing risk of an incomplete staple line. Additionally, the pursestring may tear out of the cuff during attempts to tighten the suture or the suture may break.
Cuff mobility can be accomplished by sweeping gently once the specimen has been removed from the pelvis and freeing the stump from the loose areolar tissue that surrounds it. In a traditional low anterior resection, this step is already performed, as dissection far past the level of rectal transection is necessary to ensure that the stapler can be fired with minimal firings and an adequate distal margin. Secondly, ensuring a good distal purse-string is paramount to ensure that full thickness rectum is gathered into the stapler. Finally, guiding the deployed spike of a circular stapler, through the central opening of the pursestring is vital. Alternatively, the anvil, attached to the proximal colon, can be secured to the pursestring after guiding it through the pursestring from above. Hence, the early popularity of staplers designed for hemorrhoidal surgery, which contain an extra-long anvil which facilitate this maneuver. Surgical drains have also been utilized as guide to place the spike through the pursestring center. The transanal anastomosis requires several steps, unique from the conventional approach, and should be studied and practiced. A thorough description of different transanal anastomotic techniques and their pitfalls is provided in much greater detail in another chapter.
Conclusions
TaTME is a challenging procedure, combining advanced laparoscopic skills, new planes and unfamiliar perspectives on the pelvis. Although early adopters of taTME are well within the mature portions of their learning curve, systematic learning and teaching is needed for widespread success. We have reviewed critical possible traps in the technique and provided methods to avoid these. These important technical pearls will aid the novice and intermediate surgeon in reducing the morbidity associated with the learning curve of this admittedly difficult technique.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Drs. Janindra Warusavitarne and Roel Hompes) for the series “TaTME” published in Digestive Medicine Research. The article has undergone external peer review.
Conflicts of Interest: Matthew Albert do have conflicts of interest with the current companies: Applied Medical—Stock options, consultant fees, honorarium; Conmed Surgical—Consultant fees, education, and teaching; Stryker Endoscopy—Consultant fees; Cooper Surgical—Consultant fees. The other author has no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Penna M, Hompes R, Arnold S, et al. Transanal Total Mesorectal Excision: International Registry Results of the First 720 Cases. Ann Surg 2017;266:111-7. [Crossref] [PubMed]
- Atallah S, Albert M, Monson JR. Critical concepts and important anatomic landmarks encountered during transanal total mesorectal excision (taTME): toward the mastery of a new operation for rectal cancer surgery. Tech Coloproctol 2016;20:483-94. [Crossref] [PubMed]
- Atallah S, Albert M. The neurovascular bundle of Walsh and other anatomic considerations crucial in preventing urethral injury in males undergoing transanal total mesorectal excision. Tech Coloproctol 2016;20:411-2. [Crossref] [PubMed]
- Ranbarger KR, Johnston WD, Chang JC. Prognostic significance of surgical perforation of the rectum during abdominoperineal resection for rectal carcinoma. Am J Surg 1982;143:186-8. [Crossref] [PubMed]
- Ramirez J, Aguilella V, Arribas D, et al. Transanal full-thickness excision of rectal tumours: should the defect be sutured? a randomized controlled trial. Colorectal Disease 2002;4:51-5. [Crossref] [PubMed]
- Bernardi MP, Bloemendaal AL, Albert M, et al. Transanal total mesorectal excision: dissection tips using 'O's and ‘triangles’. Tech Coloproctol 2016;20:775-8. [Crossref] [PubMed]
- Ohtani H, Tamamori Y, Azuma T, et al. A meta-analysis of the short-and long-term results of randomized controlled trials that compared laparoscopy-assisted and conventional open surgery for rectal cancer. J Gastrointest Surg 2011;15:1375-85. [Crossref] [PubMed]
- Xiong B, Ma L, Zhang C, et al. Robotic versus laparoscopic total mesorectal excision for rectal cancer: a meta-analysis. J Surg Res 2014;188:404-14. [Crossref] [PubMed]
- Denost Q, Adam J-P, Rullier A, et al. Perineal transanal approach: a new standard for laparoscopic sphincter-saving resection in low rectal cancer, a randomized trial. Ann Surg 2014;260:993-9. [Crossref] [PubMed]
- Dickson EA, Penna M, Cunningham C, et al. Carbon Dioxide Embolism Associated With Total Mesorectal Excision Surgery: A Report From the International Registries. Dis Colon Rectum 2019; [Epub ahead of print]. [Crossref]
- Andersson Å, Bergdahl L. Urologic Complications Following Abdominoperineal Resection of the Rectum. Arch Surg 1976;111:969-71. [Crossref] [PubMed]
- Atallah S, Martin-Perez B, Drake J, et al. The use of a lighted stent as a method for identifying the urethra in male patients undergoing transanal total mesorectal excision: a video demonstration. Tech Coloproctol 2015;19:375. [Crossref] [PubMed]
- Barnes TG, Volpi D, Cunningham C, et al. Improved urethral fluorescence during low rectal surgery: a new dye and a new method. Tech Coloproctol 2018;22:115-9. [Crossref] [PubMed]
- Penna M, Hompes R, Arnold S, et al. Incidence and risk factors for anastomotic failure in 1594 patients treated by transanal total mesorectal excision: results from the international TaTME registry. Ann Surg 2019;269:700-11. [Crossref] [PubMed]
Cite this article as: Albert M, Yap R. Surgical complications and pitfalls in taTME. Dig Med Res 2020;3:8.